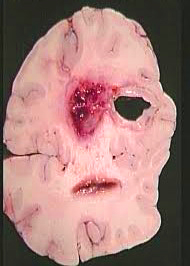
Abscess, brain (PTG)
BASIC INFORMATION
DEFINITION
A brain abscess is a focal, intracerebral infection that begins as a localized area of cerebritis and develops into a collection of pus surrounded by a well vascularized capsule.
EPIDEMIOLOGY & DEMOGRAPHICS
• Quite uncommon (occur about 2% as commonly as brain tumors)
• Occur at any age
• Peak incidences in preadolescence and middle age
• Most common source of underlying infection: contiguous spread from the paranasal sinuses, middle ear, or teeth
• Headache is usually localized to the side of the abscess, onset can be gradual or severe; present in 70% of cases.
PHYSICAL FINDINGS & CLINICAL PRESENTATION
• Classic triad: fever, headache, and focal neurologic deficit are present in <50% of cases.
• Fever is present in only 50% of patients.
• Focal neurologic findings (e.g., seizures, hemiparesis, aphasia, ataxia) depend on the location of the abscess and are seen in 30% to 50% of cases.
• Papilledema is present in 25% of cases.
• Presence of adjacent infections (dental abscess, otitis media, and sinusitis) may be a clue to the underlying diagnosis and should be sought in any suspected case.
• Time course from symptom onset to presentation ranges from hours in fulminant cases to more than 1 month; 75% present in the first 2 weeks.
• The nonspecific presentation of a brain abscess warrants that clinicians maintain a high index of suspicion.
Likely source of abscess:
A. Contiguous focus or primary infection (55% of all brain abscesses):
1. Paranasal sinus: occur in frontal lobe; streptococci, Bacteroides, Haemophilus, and Fusobacterium species
• Classic triad: fever, headache, and focal neurologic deficit are present in <50% of cases.
• Fever is present in only 50% of patients.
• Focal neurologic findings (e.g., seizures, hemiparesis, aphasia, ataxia) depend on the location of the abscess and are seen in 30% to 50% of cases.
• Papilledema is present in 25% of cases.
• Presence of adjacent infections (dental abscess, otitis media, and sinusitis) may be a clue to the underlying diagnosis and should be sought in any suspected case.
• Time course from symptom onset to presentation ranges from hours in fulminant cases to more than 1 month; 75% present in the first 2 weeks.
• The nonspecific presentation of a brain abscess warrants that clinicians maintain a high index of suspicion.
Likely source of abscess:
A. Contiguous focus or primary infection (55% of all brain abscesses):
1. Paranasal sinus: occur in frontal lobe; streptococci, Bacteroides, Haemophilus, and Fusobacterium species
2. Otitis media/mastoiditis: occur in temporal lobe and cerebellum; streptococci, Enterobacteriaceae, Bacteroides, and Pseudomonas species
3. Dental sepsis: occur in frontal lobe; mixed Fusobacterium, Bacteroides, and Streptococcus species
4. Penetrating head injury: site of abscess depends on site of wound; Staphylococcus aureus, Clostridium species, Enterobacteriaceae species
5. Postoperative: Staphylococcus epidermidis and S. aureus, Enter- obacteriaceae, and Pseudomonadaceae
B. Hematogenous spread/distant site of infection (25% of all brain abscesses): abscesses most commonly multiple, especially in middle cerebral artery distribution; infecting organisms depend on source.
1. Congenital heart disease: streptococci, Haemophilus species
2. Endocarditis: S. aureus, viridans streptococci
3. Urinary tract: Enterobacteriaceae, Pseudomonadaceae
4. Intraabdominal: streptococci, Enterobacteriaceae, anaerobes
5. Lung: streptococci, Actinomyces species, Fusobacterium species
6. Immunocompromised host: Toxoplasma species, fungi, Enterobacteriaceae, Nocardia species, tuberculosis, listeriosis
C. Cryptogenic (unknown source): 20% of all brain abscesses
3. Dental sepsis: occur in frontal lobe; mixed Fusobacterium, Bacteroides, and Streptococcus species
4. Penetrating head injury: site of abscess depends on site of wound; Staphylococcus aureus, Clostridium species, Enterobacteriaceae species
5. Postoperative: Staphylococcus epidermidis and S. aureus, Enter- obacteriaceae, and Pseudomonadaceae
B. Hematogenous spread/distant site of infection (25% of all brain abscesses): abscesses most commonly multiple, especially in middle cerebral artery distribution; infecting organisms depend on source.
1. Congenital heart disease: streptococci, Haemophilus species
2. Endocarditis: S. aureus, viridans streptococci
3. Urinary tract: Enterobacteriaceae, Pseudomonadaceae
4. Intraabdominal: streptococci, Enterobacteriaceae, anaerobes
5. Lung: streptococci, Actinomyces species, Fusobacterium species
6. Immunocompromised host: Toxoplasma species, fungi, Enterobacteriaceae, Nocardia species, tuberculosis, listeriosis
C. Cryptogenic (unknown source): 20% of all brain abscesses
DIAGNOSIS
DIFFERENTIAL DIAGNOSIS
• Other parameningeal infections: subdural empyema, epidural abscess, thrombophlebitis of the major dural venous sinuses and cortical veins
• Embolic strokes in patients with bacterial endocarditis
• Mycotic aneurysms with leakage
• Viral encephalitis (usually resulting from herpes simplex)
• Acute hemorrhagic leukoencephalitis
• Parasitic infections: toxoplasmosis, echinococcosis, cysticercosis
• Metastatic or primary brain tumors
• Cerebral infarction
• CNS vasculitis
• Chronic subdural hematoma
LABORATORY TESTS
• WBC counts are elevated in 60% of patients.
• ESR is usually elevated, but may be normal.
• Blood cultures are most often negative (10% positive).
• Lumbar puncture is contraindicated in patients with suspected abscess (20% die or suffer neurologic decline).
• The yield of Gram stain and culture of material aspirated at time of surgical drainage approaches 100%.
TREATMENT
Effective treatment involves a combination of empiric antibiotic therapy and timely excision or aspiration of the abscess.
ACUTE GENERAL Rx
• If evidence of edema or mass effect, treatment of elevated intracranial pressure is paramount (includes hyperventilation of the mechanically ventilated patient, dexamethasone, mannitol).
• Medical therapy is never a substitute for surgical intervention to relieve increased intracranial pressure.
• Steroids should be limited to patients with severe cerebral edema or midline shift.
MEDICAL Rx
Empiric antibiotic therapy guided by:
• Abscess location
• Suspicion of primary source
• Presence of single or multiple abscesses
• Patient’s underlying medical conditions (i.e., HIV, immunocompromised)
Selection of empiric antibiotic therapy:
• Primary infection or contiguous source:
1. Otitis media/mastoiditis, sinusitis, dental infection: third-generation cephalosporin (cefotaxime 2 g q6h IV or ceftriaxone 2 g q12h IV) plus metronidazole 7.5
mg/kg q6h IV or 15 mg/kg q12h IV
2. Dental infection: penicillin G 6 million units q6° plus metronidazole
3. Head trauma or postcranial surgery: third-generation cephalosporin plus metronidazole and nafcillin or vancomycin 1g q12h IV
• Hematogenous spread (congenital heart disease, endocarditis, urinary tract, lung, intraabdominal): nafcillin or vancomycin plus metronidazole plus third-generation
cephalosporin
Duration of antibiotic therapy is unclear. Most recommend parenteral treatment for 4 to 8 wek, with repeated neuroimaging to ensure adequate treatment (Imaging
suggested every wk for first 2 wk of therapy, then every 2 wk until antibiotics finished, and then every 2 to 4 mo for 1 yr to monitor for disease recurrence.)
SURGICAL Rx
• Two indicators:
1. Collect specimens for culture and sensitivity
2. Reduce mass effect
• Stereotactic biopsy or aspirate of the abscess if surgically feasible
• Essential to selection of targeted antimicrobial coverage
• Timing and choice of surgery depends on:
Primary infection source
Number and location of the abscesses
Whether the procedure is diagnostic or therapeutic
Neurologic status of the patient
DIFFERENTIAL DIAGNOSIS
• Other parameningeal infections: subdural empyema, epidural abscess, thrombophlebitis of the major dural venous sinuses and cortical veins
• Embolic strokes in patients with bacterial endocarditis
• Mycotic aneurysms with leakage
• Viral encephalitis (usually resulting from herpes simplex)
• Acute hemorrhagic leukoencephalitis
• Parasitic infections: toxoplasmosis, echinococcosis, cysticercosis
• Metastatic or primary brain tumors
• Cerebral infarction
• CNS vasculitis
• Chronic subdural hematoma
LABORATORY TESTS
• WBC counts are elevated in 60% of patients.
• ESR is usually elevated, but may be normal.
• Blood cultures are most often negative (10% positive).
• Lumbar puncture is contraindicated in patients with suspected abscess (20% die or suffer neurologic decline).
• The yield of Gram stain and culture of material aspirated at time of surgical drainage approaches 100%.
TREATMENT
Effective treatment involves a combination of empiric antibiotic therapy and timely excision or aspiration of the abscess.
ACUTE GENERAL Rx
• If evidence of edema or mass effect, treatment of elevated intracranial pressure is paramount (includes hyperventilation of the mechanically ventilated patient, dexamethasone, mannitol).
• Medical therapy is never a substitute for surgical intervention to relieve increased intracranial pressure.
• Steroids should be limited to patients with severe cerebral edema or midline shift.
MEDICAL Rx
Empiric antibiotic therapy guided by:
• Abscess location
• Suspicion of primary source
• Presence of single or multiple abscesses
• Patient’s underlying medical conditions (i.e., HIV, immunocompromised)
Selection of empiric antibiotic therapy:
• Primary infection or contiguous source:
1. Otitis media/mastoiditis, sinusitis, dental infection: third-generation cephalosporin (cefotaxime 2 g q6h IV or ceftriaxone 2 g q12h IV) plus metronidazole 7.5
mg/kg q6h IV or 15 mg/kg q12h IV
2. Dental infection: penicillin G 6 million units q6° plus metronidazole
3. Head trauma or postcranial surgery: third-generation cephalosporin plus metronidazole and nafcillin or vancomycin 1g q12h IV
• Hematogenous spread (congenital heart disease, endocarditis, urinary tract, lung, intraabdominal): nafcillin or vancomycin plus metronidazole plus third-generation
cephalosporin
Duration of antibiotic therapy is unclear. Most recommend parenteral treatment for 4 to 8 wek, with repeated neuroimaging to ensure adequate treatment (Imaging
suggested every wk for first 2 wk of therapy, then every 2 wk until antibiotics finished, and then every 2 to 4 mo for 1 yr to monitor for disease recurrence.)
SURGICAL Rx
• Two indicators:
1. Collect specimens for culture and sensitivity
2. Reduce mass effect
• Stereotactic biopsy or aspirate of the abscess if surgically feasible
• Essential to selection of targeted antimicrobial coverage
• Timing and choice of surgery depends on:
Primary infection source
Number and location of the abscesses
Whether the procedure is diagnostic or therapeutic
Neurologic status of the patient
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!