Structure of the Skin
The skin covers the entire surface of the human body. In an adult, the skin has a surface area of about 1.8 square meters (20.83 square feet). The skin is sometimes called the cutaneous membrane or the integument. Because the skin has several accessory organs, it is also possible to speak of the integumentary system. The skin (Fig. 5.1) has two regions: the epidermis and the dermis. The hypodermis, a subcutaneous tissue, is found between the skin and any underlying structures, such as muscle. Usually, the hypodermis is only loosely attached to underlying muscle tissue, but where no muscles are present, the hypodermis attaches directly to bone. For example, there are flexion creases where the skin attaches directly to the joints of the fingers.
Epidermis
The epidermis is the outer and thinner region of the skin. It is made up of stratified squamous epithelium divided into several layers; the deepest layer is the stratum basale, and the most superficial layer is the stratum corneum.
Stratum Basale
The basal cells of the stratum basale lie just superior to the dermis and are constantly dividing and producing new cells that are pushed to the surface of the epidermis in two to four weeks. As the cells move away from the dermis, they get progressively farther away from the blood vessels in the dermis. Because these cells are not being supplied with nutrients and oxygen (the epidermis itself lacks blood vessels), they eventually die and are sloughed off.
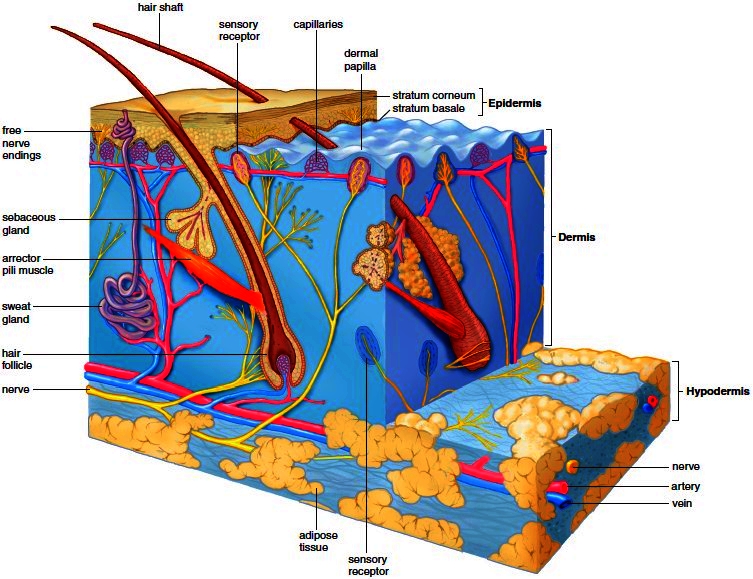
Figure 5.1 Skin anatomy. Skin is composed of two regions: the epidermis and the dermis. The hypodermis, or subcutaneous layer, is located beneath the skin.
Langerhans cells are macrophages found deep in the epidermis. Macrophages are related to monocytes, white blood cells produced in red bone marrow. These cells phagocytize microbes and then travel to lymphatic organs, where they stimulate the immune system to react.
Melanocytes are another type of specialized cell located in the deeper epidermis. Melanocytes produce melanin, the pigment primarily responsible for skin color. Since the number of melanocytes is about the same in all individuals, variation in skin color is due to the amount of melanin produced and its distribution. When skin is exposed to the sun, melanocytes produce more melanin to protect the skin from the damaging effects of the ultraviolet (UV) radiation in sunlight. The melanin is passed to other epidermal cells, and the result is tanning, or in some people, the formation of patches of melanin called freckles. A hereditary trait characterized by the lack of ability to produce melanin is known as albinism. Individuals with this disorder lack pigment not only in the skin, but also in the hair and eyes. Another pigment, called carotene, is present in epidermal cells and in the dermis and gives the skin of certain Asians its yellowish hue. The pinkish color of fair-skinned people is due to the pigment hemoglobin in the red blood cells in the capillaries of the dermis.
Stratum Corneum
As cells are pushed toward the surface of the skin, they become flat and hard, forming the tough, uppermost layer of the epidermis, the stratum corneum. Hardening is caused by keratinization, the cellular production of a fibrous, waterproof protein called keratin. Over much of the body, keratinization is minimal, but the palms of the hands and the soles of the feet normally have a particularly thick outer layer of dead, keratinized cells. The waterproof nature of keratin protects the body from water loss and water gain. The stratum corneum allows us to live in a desert or a tropical rain forest without damaging our inner cells. The stratum corneum also serves as a mechanical barrier against microbe invasion. This protective function of skin is assisted by the secretions of sebaceous glands, which weaken or kill bacteria on the skin.
Dermis
The dermis, a deeper and thicker region than the epidermis, is composed of dense irregular connective tissue. The upper layer of the dermis has fingerlike projections called dermal papillae. Dermal papillae project into and anchor the epidermis. In the overlying epidermis, dermal papillae cause ridges, resulting in spiral and concentric patterns commonly known as “fingerprints.” The function of the epidermal ridges is to increase friction and thus provide a better gripping surface. Because they are unique to each person, fingerprints and footprints can be used for identification purposes.
The dermis contains collagenous and elastic fibers. The collagenous fibers are flexible but offer great resistance to overstretching; they prevent the skin from being torn. The elastic fibers stretch to allow movement of underlying muscles and joints, but they maintain normal skin tension. The dermis also contains blood vessels that nourish the skin. Blood rushes into these vessels when a person blushes; blood is reduced in them when a person turns cyanotic, or “blue.” Sometimes, blood flow to a particular area is restricted in bedridden patients, and consequently they develop decubitus ulcers (bedsores) (Fig. 5.2). These can be prevented by changing the patient’s position frequently and by massaging the skin to stimulate blood flow. There are also numerous sensory nerve fibers in the dermis that take nerve impulses to and from the accessory structures of the skin.
Hypodermis
Hypodermis, or subcutaneous tissue, lies below the dermis. From the names for this layer, we get the terms subcutaneous injection, performed with a hypodermic needle.
Melanocytes are another type of specialized cell located in the deeper epidermis. Melanocytes produce melanin, the pigment primarily responsible for skin color. Since the number of melanocytes is about the same in all individuals, variation in skin color is due to the amount of melanin produced and its distribution. When skin is exposed to the sun, melanocytes produce more melanin to protect the skin from the damaging effects of the ultraviolet (UV) radiation in sunlight. The melanin is passed to other epidermal cells, and the result is tanning, or in some people, the formation of patches of melanin called freckles. A hereditary trait characterized by the lack of ability to produce melanin is known as albinism. Individuals with this disorder lack pigment not only in the skin, but also in the hair and eyes. Another pigment, called carotene, is present in epidermal cells and in the dermis and gives the skin of certain Asians its yellowish hue. The pinkish color of fair-skinned people is due to the pigment hemoglobin in the red blood cells in the capillaries of the dermis.
Stratum Corneum
As cells are pushed toward the surface of the skin, they become flat and hard, forming the tough, uppermost layer of the epidermis, the stratum corneum. Hardening is caused by keratinization, the cellular production of a fibrous, waterproof protein called keratin. Over much of the body, keratinization is minimal, but the palms of the hands and the soles of the feet normally have a particularly thick outer layer of dead, keratinized cells. The waterproof nature of keratin protects the body from water loss and water gain. The stratum corneum allows us to live in a desert or a tropical rain forest without damaging our inner cells. The stratum corneum also serves as a mechanical barrier against microbe invasion. This protective function of skin is assisted by the secretions of sebaceous glands, which weaken or kill bacteria on the skin.
Dermis
The dermis, a deeper and thicker region than the epidermis, is composed of dense irregular connective tissue. The upper layer of the dermis has fingerlike projections called dermal papillae. Dermal papillae project into and anchor the epidermis. In the overlying epidermis, dermal papillae cause ridges, resulting in spiral and concentric patterns commonly known as “fingerprints.” The function of the epidermal ridges is to increase friction and thus provide a better gripping surface. Because they are unique to each person, fingerprints and footprints can be used for identification purposes.
The dermis contains collagenous and elastic fibers. The collagenous fibers are flexible but offer great resistance to overstretching; they prevent the skin from being torn. The elastic fibers stretch to allow movement of underlying muscles and joints, but they maintain normal skin tension. The dermis also contains blood vessels that nourish the skin. Blood rushes into these vessels when a person blushes; blood is reduced in them when a person turns cyanotic, or “blue.” Sometimes, blood flow to a particular area is restricted in bedridden patients, and consequently they develop decubitus ulcers (bedsores) (Fig. 5.2). These can be prevented by changing the patient’s position frequently and by massaging the skin to stimulate blood flow. There are also numerous sensory nerve fibers in the dermis that take nerve impulses to and from the accessory structures of the skin.
Hypodermis
Hypodermis, or subcutaneous tissue, lies below the dermis. From the names for this layer, we get the terms subcutaneous injection, performed with a hypodermic needle.
Figure 5.2 A decubitus ulcer (bedsore). The most frequent sites for bedsores are in the skin overlying a bony projection, such as on the hip, ankle, heel, shoulder, or elbow.

The hypodermis is composed of loose connective tissue, including adipose (fat) tissue. Fat is an energy storage form that can be called upon when necessary to supply the body with molecules for cellular respiration. Adipose tissue also helps insulate the body. A well-developed hypodermis gives the body a rounded appearance and provides protective padding against external assaults. Excessive development of adipose tissue in the hypodermis layer results in obesity.
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!