Table 18.1 Nomenclature of bone tumors
Breech birth
BASIC INFORMATION
DEFINITION
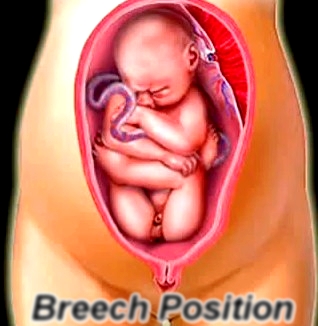
Breech presentation exists when the fetal longitudinal axis is such that the cephalic pole occupies the uterine fundus. Three types exist, with respective percentages at term, frank (50% to 75%, flexed hips, extended thighs), complete (4.8% to 11.8%, flexed hips and knees), and footling (14% to 40%, hips extended).
EPIDEMIOLOGY & DEMOGRAPHICS
INCIDENCE: Gestational age dependent: 4% to 5% overall, 15% at 29 to 32 weeks, 33% at 21 to 24 weeks
PERINATAL MORTALITY: 10% to 23%, or three to five times increase over vertex presentation at term. If one corrects for the associated increase in congenital anomalies and complications of prematurity, the morbidity and mortality approach that of the vertex presentation at term regardless of route of delivery.
PHYSICAL FINDINGS & CLINICAL PRESENTATION
• Maintain a high index of suspicion
• Lack of presenting part on vaginal examination
• Fetal heart tones heard above the umbilicus
• Leopold maneuvers revealing mobile fetal part in the uterine fundus
ETIOLOGY
• Abnormal placentation (fundal), uterine anomalies (fibroids, septa), pelvic or adnexal masses, alterations in fetal muscular tone, or fetal malformations
• Associated conditions: trisomy 13, 18, 21, Potter syndrome, myotonic dystrophy, prematurity
DIAGNOSIS
DIFFERENTIAL DIAGNOSIS
Vertex, oblique, or transverse lie
WORKUP
• If possible, determine reason for breech presentation, history of uterine anomalies, gestational age, or associated fetal congenital anomalies.
• Assess fetal status, by either continuous fetal heart rate monitoring or ultrasound.
• Assess pelvis to determine feasibility of vaginal delivery.
• Assess risk for safety of vaginal vs. abdominal delivery.
IMAGING STUDIES
Ultrasound to evaluate for:
• Fetal anomalies, such as hydrocephalus
• Placental location
• Position of fetal head relative to spine (check for hyperextension)
• Estimated fetal weight (2500 to 3800 grams)
• Type of breech (frank, complete, footling)
CRITERIA FOR TRIAL OF LABOR
• Estimated fetal weight 2000 to 3800 grams
• Frank breech
• Adequate pelvis
• Flexed fetal head
• Continuous fetal monitoring
• Normal progress of labor
• Bedside availability of anesthesia and capability for immediate C-section
• Informed consent
• Obstetrician trained in vaginal breech delivery
CRITERIA FOR C-SECTION
• Estimated fetal weight <1500 grams or >4000 grams
• Footling presentation (22% risk of cord prolapse, usually late in course of labor)
• Inadequate pelvis
• Hyperextended fetal head (24% risk of spinal cord injury)
• Nonreassuring fetal status
• Abnormal progress of labor
• Lack of trained obstetrician
TREATMENT
ACUTE GENERAL Rx
• Vaginal delivery in selected patient: allow maternal expulsive forces to deliver fetus until scapula visible (avoiding traction); with flexion and/or Piper forceps, deliver fetal head.
• Perform C-section for the above-mentioned reasons.
• External cephalic version, success 60% to 75%, after 37 weeks, contraindicated with placental abruption, low-lying placenta, maternal hypertension, previous uterine incision, multiple gestation, nonreassuring fetal status.
• Adequate pelvic/cervical relaxation essential for vaginal breech (i.e., need anesthesia in-room during birth [delivery] with uterine relaxants on hand [NTG, terbutaline])
COMPLICATIONS
• Head entrapment: leading cause of death (with the exception of anomalous fetuses), 88 cases/1000 deliveries, avoid by maintaining flexion of fetal head, use of Piper forceps or Dührssen’s incisions. Before 36 weeks, HC > AC, thus fetal predisposition. Tentorial tears secondary to hyperextended head. Association with trisomy 22 in 4% to 5% of cases. Avoid hyperextension of head during delivery.

Breech birth demonstration using the clinical simulation suite.

• Cord prolapse: usually occurs late in the course of labor. Incidence depends on type of breech-frank (0.5%), complete (4% to 5%), footling (10%).
• Nuchal arm: arm extended above fetal head, occurs when there is undue traction before delivery of fetal scapulas. Treatment depends on bringing trapped arm across infant’s face.
DISPOSITION
If confounding variables are corrected for, such as prematurity and associated congenital anomalies (6.3% of breeches vs. 2.4% in general population), route of delivery plays a less important role in fetal outcome than previously thought.
REFERRAL
An obstetrician trained in delivery of the vaginal breech is a prerequisite for attempting vaginal route, although it must be explained to the patient that with C-section certain risks (such as hyperextension of the fetal head with resultant spinal cord injury) may be minimized but not eliminated.
• Nuchal arm: arm extended above fetal head, occurs when there is undue traction before delivery of fetal scapulas. Treatment depends on bringing trapped arm across infant’s face.
DISPOSITION
If confounding variables are corrected for, such as prematurity and associated congenital anomalies (6.3% of breeches vs. 2.4% in general population), route of delivery plays a less important role in fetal outcome than previously thought.
REFERRAL
An obstetrician trained in delivery of the vaginal breech is a prerequisite for attempting vaginal route, although it must be explained to the patient that with C-section certain risks (such as hyperextension of the fetal head with resultant spinal cord injury) may be minimized but not eliminated.
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!