Table 18.1 Nomenclature of bone tumors
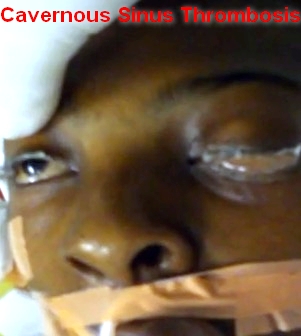
Cavernous sinus thrombosis
BASIC INFORMATION
DEFINITION
Cavernous sinus thrombosis is an uncommon diagnosis usually stemming from infections of the face or paranasal sinuses resulting in thrombosis of the cavernous sinus and inflammation of its surrounding anatomic structures, including cranial nerves III, IV, V (ophthalmic and maxillary branch), and VI, and the internal carotid artery.
SYNONYMS
Intracranial venous sinus thrombosis or thrombophlebitis
EPIDEMIOLOGY & DEMOGRAPHICS
• Cavernous sinus thrombosis is rare.
• Before antibiotics the mortality rate from cavernous sinus thrombosis was 85% to 100%.
• With antibiotics, the mortality rates range between 25% and 35%.
• Morbidity remains high (between 20% and 50%).
PHYSICAL FINDINGS & CLINICAL PRESENTATION
The classic findings include:
• Ptosis
• Proptosis
• Chemosis
• Cranial nerve palsies (III, IV, V, VI)
1. Sixth nerve palsy is the most common.
2. Sensory deficits of the ophthalmic and maxillary branch of the fifth nerve are common.
Other findings:
• Decreased visual acuity and blindness may occur.
• Venous engorgement and papilledema on funduscopic examination may be found.
• Fever, tachycardia, sepsis may be present.
• Headache with nuchal rigidity may occur.
• Pupil may be dilated and sluggishly reactive.
ETIOLOGY
• Staphylococcus aureus is the most common infectious microbe, found in 55% to 65% of the cases.
• Streptococcus is the second leading cause.
• Gram-negative rods and anaerobes may also lead to cavernous sinus thrombosis.
• The most common primary site of infection leading to cavernous sinus thrombosis is sphenoid sinusitis; however, other sites of infection, including the middle ear, orbit, eye, eyelid, and face, can result in the same sequelae.
DIAGNOSIS
• The diagnosis of cavernous sinus thrombosis is made clinically.
• Proptosis, ptosis, chemosis, and cranial nerve palsy beginning in one eye and progressing to the other eye establish the diagnosis.
DIFFERENTIAL DIAGNOSIS
• Orbital cellulitis
• Internal carotid artery aneurysm
• CVA
• Migraine headache
• Allergic blepharitis
• Thyroid exophthalmos
• Brain tumor
• Meningitis
• Mucormycosis
• Trauma
WORKUP
Cavernous sinus thrombosis is a clinical diagnosis with laboratory tests and imaging studies confirming the clinical impression.
LABORATORY TESTS
• CBC, ESR, blood cultures, and sinus cultures help establish and identify an infectious primary source.
• Lumbar puncture is necessary to rule out meningitis.
IMAGING STUDIES
• Sinus films are helpful in the diagnosis of sphenoid sinusitis. Opacification, sclerosis, and air-fluid levels are typical findings.
• CT scan is the best study to diagnose sphenoid sinusitis; however, CT scan is not very sensitive in diagnosing cavernous sinus thrombosis.
• MRI is the imaging study of choice to diagnose cavernous sinus thrombosis.
• Cerebral angiography can be performed, but it is invasive and not very sensitive.
• Orbital venography is difficult to perform, but it is excellent in diagnosing occlusion of the cavernous sinus.
TREATMENT
NONPHARMACOLOGIC THERAPY
Recognizing the primary source of infection (e.g., facial cellulitis, middle ear, and sinus infections) and treating the primary source expeditiously is the best way to prevent cavernous sinus thrombosis.
ACUTE GENERAL Rx
• Broad-spectrum intravenous antibiotics are used until a definite pathogen is found.
1. Nafcillin 1.5 g IV q4h
• The diagnosis of cavernous sinus thrombosis is made clinically.
• Proptosis, ptosis, chemosis, and cranial nerve palsy beginning in one eye and progressing to the other eye establish the diagnosis.
DIFFERENTIAL DIAGNOSIS
• Orbital cellulitis
• Internal carotid artery aneurysm
• CVA
• Migraine headache
• Allergic blepharitis
• Thyroid exophthalmos
• Brain tumor
• Meningitis
• Mucormycosis
• Trauma
WORKUP
Cavernous sinus thrombosis is a clinical diagnosis with laboratory tests and imaging studies confirming the clinical impression.
LABORATORY TESTS
• CBC, ESR, blood cultures, and sinus cultures help establish and identify an infectious primary source.
• Lumbar puncture is necessary to rule out meningitis.
IMAGING STUDIES
• Sinus films are helpful in the diagnosis of sphenoid sinusitis. Opacification, sclerosis, and air-fluid levels are typical findings.
• CT scan is the best study to diagnose sphenoid sinusitis; however, CT scan is not very sensitive in diagnosing cavernous sinus thrombosis.
• MRI is the imaging study of choice to diagnose cavernous sinus thrombosis.
• Cerebral angiography can be performed, but it is invasive and not very sensitive.
• Orbital venography is difficult to perform, but it is excellent in diagnosing occlusion of the cavernous sinus.
TREATMENT
NONPHARMACOLOGIC THERAPY
Recognizing the primary source of infection (e.g., facial cellulitis, middle ear, and sinus infections) and treating the primary source expeditiously is the best way to prevent cavernous sinus thrombosis.
ACUTE GENERAL Rx
• Broad-spectrum intravenous antibiotics are used until a definite pathogen is found.
1. Nafcillin 1.5 g IV q4h
2. Cefotaxime 1.5 to 2 g IV q4h
3. Metronidazole 15 mg/kg load followed by 7.5 mg/kg IV q6h
• Anticoagulation with heparin is controversial. Retrospective studies show conflicting data. This decision should be made with subspecialty consultation.
• Steroid therapy is also controversial.
CHRONIC Rx
Surgical drainage with sphenoidotomy is indicated if the primary site of infection is thought to be the sphenoid sinus.
DISPOSITION
• Cavernous sinus thrombosis can be a life-threatening, rapidly progressive infectious disease with high morbidity and mortality rates despite antibiotic use.
• Complications in treated patients include oculomotor weakness, blindness, pituitary insufficiency, and hemiparesis.
REFERRAL
If the diagnosis is suspected, this should be considered a medical emergency. Depending on the primary site of infection, appropriate consultation should be made (e.g., ENT, ophthalmology, and infectious disease.)
3. Metronidazole 15 mg/kg load followed by 7.5 mg/kg IV q6h
• Anticoagulation with heparin is controversial. Retrospective studies show conflicting data. This decision should be made with subspecialty consultation.
• Steroid therapy is also controversial.
CHRONIC Rx
Surgical drainage with sphenoidotomy is indicated if the primary site of infection is thought to be the sphenoid sinus.
DISPOSITION
• Cavernous sinus thrombosis can be a life-threatening, rapidly progressive infectious disease with high morbidity and mortality rates despite antibiotic use.
• Complications in treated patients include oculomotor weakness, blindness, pituitary insufficiency, and hemiparesis.
REFERRAL
If the diagnosis is suspected, this should be considered a medical emergency. Depending on the primary site of infection, appropriate consultation should be made (e.g., ENT, ophthalmology, and infectious disease.)
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!