Table 18.1 Nomenclature of bone tumors
Chancroid
BASIC INFORMATION
DEFINITION
Chancroid is a sexually transmitted disease characterized by painful genital ulceration and inflammatory inguinal adenopathy.
Chancroid or soft chancre is an acute STI caused by Haemophilus ducreyi. Although a less common cause of genital ulceration than HSV-2, it is prevalent in parts of Africa and Asia. It is rare in the UK with cases usually associated with travel to or partners from endemic areas. Epidemiological studies in Africa have shown an association between genital ulcer disease, frequently chancroid and the acquisition of HIV infection. A new urgency to control chancroid has resulted from these observations.
SYNONYMS
Soft chancre
Ulcus molle
Clinical features
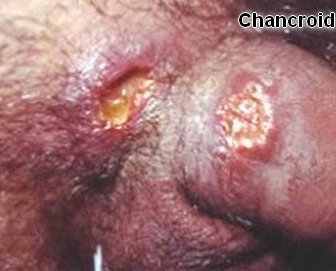
The incubation period is 3-10 days. At the site of inoculation an erythematous papular lesion forms which then breaks down into an ulcer. The ulcer frequently has a necrotic base, a ragged edge, bleeds easily and is painful. Several ulcers may merge to form giant serpiginous lesions. Ulcers appear most commonly on the prepuce and frenulum in men and can erode through tissues. In women the most commonly affected site is the vaginal entrance and the perineum and lesions sometimes go unnoticed. At the same time, inguinal lymphadenopathy develops (usually unilateral) and can progress to form large buboes which suppurate.
EPIDEMIOLOGY & DEMOGRAPHICS
• Exact incidence is unknown.
• Occurs more frequently in men (male:female ratio of 10:1).
• Clinical infection is rare in women.
• There is a higher incidence in uncircumcised men and in tropical and subtropical regions.
• Incubation period is 4 to 7 days but may take up to 3 weeks.
• High incidence of HIV infection associated with chancroid.
PHYSICAL FINDINGS & CLINICAL PRESENTATION
• One to three extremely painful ulcers, accompanied by tender inguinal lymphadenopathy (especially if fluctuant)
• May present with inguinal bubo and several ulcers
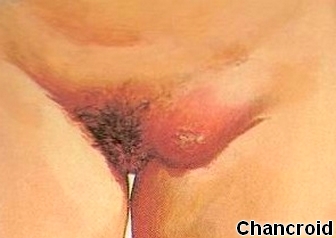
• In women: initial lesion in the fourchette, labia minora, urethra, cervix, or anus; inflammatory pustule or papule that ruptures leaving a shallow, nonindurated shallow ulceration, usually 1- to 2-cm diameter with ragged, undermined edges
• Unilateral lymphadenopathy develops 1 week later in 53% of patients
ETIOLOGY
Haemophilus ducreyi, a bacillus
DIAGNOSIS
DIFFERENTIAL DIAGNOSIS
Chancroid must be differentiated from other genital ulcer diseases. Co-infection with syphilis and herpes simplex is common. Isolation of H. ducreyi, a fastidious organism, in specialized culture media is definitive but difficult. Swabs should be taken from the ulcer and material aspirated from the local lymph nodes for culture. Polymerase chain reaction (PCR) techniques are available. Gram stains of clinical material may show characteristic coccobacilli, but this is an insensitive test. Detection of antibody to H ducreyi using EIA may be useful for population surveillance but, at an individual level, lacks sensitivity and specificity. A ‘probable diagnosis’, may be made if the patient has the appropriate clinical picture, without evidence of T. pallidum or herpes simplex infection.
WORKUP
• Diagnosis based on history and physical examination is often inadequate. Must rule out syphilis in women because of the consequences of inappropriate therapy in pregnant women. Base initial diagnosis and treatment recommendations on clinical impression of appearance of ulcer and most likely diagnosis for population. Definitive diagnosis is made by isolation of organism from ulcers by culture or Gram stain.
LABORATORY TESTS
Darkfield microscopy, RPR, HSV cultures, H. ducreyi culture, HIV testing recommended
TREATMENT
NONPHARMACOLOGIC THERAPY
Fluctuant nodes should be aspirated through healthy adjacent skin to prevent formation of draining sinus. I&D not recommended, delays healing. Use warm compresses to remove necrotic material.
ACUTE GENERAL Rx
• Azithromycin 1 g PO (single dose) or
• Ceftriaxone 250 mg IM (single dose) or
• Ciprofloxacin 500 mg PO bid for 3 days or
• Erythromycin 500 mg PO qid for 7 days
NOTE: Ciprofloxacin is contraindicated in patients who are pregnant, lactating, or less than 18 years of age.
• HIV-infected patients may need more prolonged therapy
DISPOSITION
• All sexual partners should be treated with a 10-day course of one of the above regimens.
• Patients should be reexamined 3 to 7 days after initiation of therapy. Ulcers should improve symptomatically within 3 days and objectively within 7 days after initiation of successful therapy.
DIFFERENTIAL DIAGNOSIS
Chancroid must be differentiated from other genital ulcer diseases. Co-infection with syphilis and herpes simplex is common. Isolation of H. ducreyi, a fastidious organism, in specialized culture media is definitive but difficult. Swabs should be taken from the ulcer and material aspirated from the local lymph nodes for culture. Polymerase chain reaction (PCR) techniques are available. Gram stains of clinical material may show characteristic coccobacilli, but this is an insensitive test. Detection of antibody to H ducreyi using EIA may be useful for population surveillance but, at an individual level, lacks sensitivity and specificity. A ‘probable diagnosis’, may be made if the patient has the appropriate clinical picture, without evidence of T. pallidum or herpes simplex infection.
WORKUP
• Diagnosis based on history and physical examination is often inadequate. Must rule out syphilis in women because of the consequences of inappropriate therapy in pregnant women. Base initial diagnosis and treatment recommendations on clinical impression of appearance of ulcer and most likely diagnosis for population. Definitive diagnosis is made by isolation of organism from ulcers by culture or Gram stain.
LABORATORY TESTS
Darkfield microscopy, RPR, HSV cultures, H. ducreyi culture, HIV testing recommended
TREATMENT
NONPHARMACOLOGIC THERAPY
Fluctuant nodes should be aspirated through healthy adjacent skin to prevent formation of draining sinus. I&D not recommended, delays healing. Use warm compresses to remove necrotic material.
ACUTE GENERAL Rx
• Azithromycin 1 g PO (single dose) or
• Ceftriaxone 250 mg IM (single dose) or
• Ciprofloxacin 500 mg PO bid for 3 days or
• Erythromycin 500 mg PO qid for 7 days
NOTE: Ciprofloxacin is contraindicated in patients who are pregnant, lactating, or less than 18 years of age.
• HIV-infected patients may need more prolonged therapy
DISPOSITION
• All sexual partners should be treated with a 10-day course of one of the above regimens.
• Patients should be reexamined 3 to 7 days after initiation of therapy. Ulcers should improve symptomatically within 3 days and objectively within 7 days after initiation of successful therapy.
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!