Function of the Heart
Although the heart’s right and left sides are separated from each other, they work together. Blood is squeezed through the chambers by a heart muscle contraction that begins in the thin-walled upper chambers, the atria, and is followed by a contraction of the thick muscle of the lower chambers, the ventricles. This active phase is called systole, and in each case, it is followed by a resting period known as diastole. One complete sequence of heart contraction and relaxation is called the cardiac cycle (Fig. 10-10). Each cardiac cycle represents a single heartbeat. At rest, one cycle takes an average of 0.8 seconds. The contraction phase of the cardiac cycle begins with contraction of both atria, which forces blood through the AV valves into the ventricles. The atrial walls are thin, and their contractions are not very powerful. However, they do improve the heart’s efficiency by forcing blood into the ventricles before these lower chambers contract. Atrial contraction is completed at the time ventricular contraction begins. Thus, a resting phase (diastole) begins in the atria at the same time that a contraction (systole) begins in the ventricles. After the ventricles have contracted, all chambers are relaxed for a short period as they fill with blood. Then another cycle begins with an atrial contraction followed by a ventricular contraction. Although both upper and lower chambers have a systolic and diastolic phase in each cardiac cycle, discussions of heart function usually refer to these phases as they occur in the ventricles, because these chambers contract more forcefully and drive blood into the arteries.

Figure 10-10 The cardiac cycle.
Cardiac Output
A unique property of heart muscle is its ability to adjust the strength of contraction to the amount of blood received. When the heart chamber is filled and the wall stretched (within limits), the contraction is strong. As less blood enters the heart, contractions become less forceful. Thus, as more blood enters the heart, as occurs during exercise, the muscle contracts with greater strength to push the larger volume of blood out into the blood vessels. The volume of blood pumped by each ventricle in 1 minute is termed the cardiac output (CO). It is the product of the stroke volume (SV)-the volume of blood ejected from the ventricle with each beat-and the heart rate (HR)-the number of times the heart beats per minute.
The Heart’s Conduction System
Like other muscles, the heart muscle is stimulated to contract by a wave of electrical energy that passes along the cells. This action potential is generated by specialized tissue within the heart and spreads over structures that form the heart’s conduction system (Fig. 10-11). Two of these structures are tissue masses called nodes, and the remainder consists of specialized fibers that branch through the myocardium. The sinoatrial (SA) node is located in the upper wall of the right atrium in a small depression described as a sinus. This node initiates the heartbeats by generating an action potential at regular intervals. Because the SA node sets the rate of heart contractions, it is commonly called the pacemaker. The second node, located in the interatrial septum at the bottom of the right atrium, is called the atrioventricular (AV) node. The atrioventricular bundle, also known as the bundle of His, is located at the top of the interventricular septum. It has branches that extend to all parts of the ventricular walls. Fibers travel first down both sides of the interventricular septum in groups called the right and left bundle branches. Smaller Purkinje fibers, also called conduction myofibers, then travel in a branching network throughout the myocardium of the ventricles. Intercalated disks allow the rapid flow of impulses throughout the heart muscle.

Figure 10-11 Conduction system of the heart. The sinoatrial (SA) node, the atrioventricular (AV) node, and specialized fibers conduct the electrical energy that stimulates the heart muscle to contract.
The Conduction Pathway
The order in which impulses travel through the heart is as follows:1. The sinoatrial node generates the electrical impulse that begins the heartbeat (see Fig. 10-11).
2. The excitation wave travels throughout the muscle of each atrium, causing the atria to contract. At the same time, impulses also travel directly to the AV node by means of fibers in the wall of the atrium that make up the internodal pathways.
3. The atrioventricular node is stimulated. A relatively slower rate of conduction through the AV node allows time for the atria to contract and complete the filling of the ventricles before the ventricles contract.
4. The excitation wave travels rapidly through the bundle of His and then throughout the ventricular walls by means of the bundle branches and Purkinje fibers. The entire ventricular musculature contracts almost at the same time.
A normal heart rhythm originating at the SA node is termed a sinus rhythm. As a safety measure, a region of the conduction system other than the sinoatrial node can generate a heartbeat if the sinoatrial node fails, but it does so at a slower rate.
Control of the Heart Rate
Although the heart’s fundamental beat originates within the heart itself, the heart rate can be influenced by the nervous system, hormones and other factors in the internal environment. The autonomic nervous system (ANS) plays a major role in modifying the heart rate according to need (Fig. 10- 12). Sympathetic nervous system stimulation increases the heart rate.
During a fight-or-flight response, the sympathetic nerves can boost the cardiac output two to three times the resting value. Sympathetic fibers increase the contraction rate by stimulating the SA and AV nodes. They also increase the contraction force by acting directly on the fibers of the myocardium. These actions translate into increased cardiac output. Parasympathetic stimulation decreases the heart rate to restore homeostasis. The parasympathetic nerve that supplies the heart is the vagus nerve (cranial nerve X). It slows the heart rate by acting on the SA and AV nodes. These ANS influences allow the heart to meet changing needs rapidly. The heart rate is also affected by substances circulating in the blood, including hormones, ions, and drugs. Regular exercise strengthens the heart and increases the amount of blood ejected with each beat. Consequently, the circulatory needs of the body at rest can be met with a lower heart rate. Trained athletes usually have a low resting heart rate.
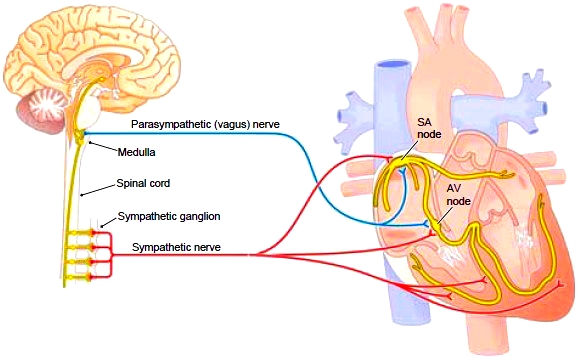
Figure 10-12 Autonomic nervous system regulation of the heart. The ANS affects the rate and force of heart contractions.
Variations in Heart Rates
* Bradycardia is a relatively slow heart rate of less than 60 beats/ minute. During rest and sleep, the heart may beat less than 60 beats/minute, but the rate usually does not fall below 50 beats/minute.
* Tachycardia refers to a heart rate of more than 100 beats/minute. Tachycardia is normal during exercise or stress but may also occur under abnormal conditions.
* Bradycardia is a relatively slow heart rate of less than 60 beats/ minute. During rest and sleep, the heart may beat less than 60 beats/minute, but the rate usually does not fall below 50 beats/minute.
* Tachycardia refers to a heart rate of more than 100 beats/minute. Tachycardia is normal during exercise or stress but may also occur under abnormal conditions.
* Sinus arrhythmia is a regular variation in heart rate caused by changes in the rate and depth of breathing. It is a normal phenomenon.
* Premature beat, also called extrasystole, is a beat that comes before the expected normal beat. In healthy people, they may be initiated by caffeine, nicotine, or psychological stresses. They are also common in people with heart disease.
Heart Sounds
The normal heart sounds are usually described by the syllables “lubb” and “dupp.” The first, “lubb,” is a longer, lower-pitched sound that occurs at the start of ventricular systole. It is probably caused by a combination of events, mainly closure of the atrioventricular valves. This action causes vibrations in the blood passing through the valves and in the tissue surrounding the valves. The second, or “dupp,” sound is shorter and sharper. It occurs at the beginning of ventricular relaxation and is caused largely by sudden closure of the semilunar valves.
Murmurs An abnormal sound is called a murmur and is usually due to faulty action of a valve. For example, if a valve fails to close tightly and blood leaks back, a murmur is heard. Another condition giving rise to an abnormal sound is the narrowing (stenosis) of a valve opening. The many conditions that can cause abnormal heart sounds include congenital (birth) defects, disease, and physiologic variations. An abnormal sound caused by any structural change in the heart or the vessels connected with the heart is called an organic murmur. Certain normal sounds heard while the heart is working may also be described as murmurs, such as the sound heard during rapid filling of the ventricles. To differentiate these from abnormal sounds, they are more properly called functional murmurs.
* Premature beat, also called extrasystole, is a beat that comes before the expected normal beat. In healthy people, they may be initiated by caffeine, nicotine, or psychological stresses. They are also common in people with heart disease.
Heart Sounds
The normal heart sounds are usually described by the syllables “lubb” and “dupp.” The first, “lubb,” is a longer, lower-pitched sound that occurs at the start of ventricular systole. It is probably caused by a combination of events, mainly closure of the atrioventricular valves. This action causes vibrations in the blood passing through the valves and in the tissue surrounding the valves. The second, or “dupp,” sound is shorter and sharper. It occurs at the beginning of ventricular relaxation and is caused largely by sudden closure of the semilunar valves.
Murmurs An abnormal sound is called a murmur and is usually due to faulty action of a valve. For example, if a valve fails to close tightly and blood leaks back, a murmur is heard. Another condition giving rise to an abnormal sound is the narrowing (stenosis) of a valve opening. The many conditions that can cause abnormal heart sounds include congenital (birth) defects, disease, and physiologic variations. An abnormal sound caused by any structural change in the heart or the vessels connected with the heart is called an organic murmur. Certain normal sounds heard while the heart is working may also be described as murmurs, such as the sound heard during rapid filling of the ventricles. To differentiate these from abnormal sounds, they are more properly called functional murmurs.
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!