Circulation and the Heart
The next two chapters investigate how the blood delivers oxygen and nutrients to the cells and carries away the waste products of cell metabolism. The continuous oneway circuit of blood through the body in the blood vessels is known as the circulation. The prime mover that propels blood throughout the body is the heart. This page examines the structure and function of the heart to lay the foundation for the detailed discussion of blood vessels that follows. The importance of the heart has been recognized for centuries. Strokes (the contractions) of this pump average about 72 per minute and are carried on unceasingly for the whole of a lifetime. The beating of the heart is affected by the emotions, which may explain the frequent references to it in song and poetry. However, the vital functions of the heart and its disorders are of more practical concern.
Location of the Heart
The heart is slightly bigger than a person’s fist. This organ is located between the lungs in the center and a bit to the left of the midline of the body (Fig. 10-1). It occupies most of the mediastinum, the central region of the thorax. The heart’s apex, the pointed, inferior portion, is directed toward the left. The broad, superior base is the area of attachment for the large vessels carrying blood into and out of the heart.

Figure 10-1 The heart in position in the thorax (anterior view).
Structure of the Heart
The heart is a hollow organ, with walls formed of three different layers. Just as a warm coat might have a smooth lining, a thick and bulky interlining, and an outer layer of a third fabric, so the heart wall has three tissue layers (Fig. 10-2). Starting with the innermost layer, these are as follows:
* The endocardium is a thin, smooth layer of epithelial cells that lines the heart’s interior. The endocardium provides a smooth surface for easy flow as blood travels through the heart. Extensions of this membrane cover the flaps (cusps) of the heart valves.
* The myocardium, the heart muscle, is the thickest layer and pumps blood through the vessels. Cardiac muscle’s unique structure is described in more detail next.
* The epicardium is a serous membrane that forms the thin, outermost layer of the heart wall.
The Pericardium
The pericardium is the sac that encloses the heart (Fig. 10-2). The outermost and heaviest layer of this sac is the fibrous pericardium. Connective tissue anchors this pericardial layer to the diaphragm, located inferiorly; the sternum, located anteriorly; and to other structures surrounding the heart, thus holding the heart in place.
The heart is a hollow organ, with walls formed of three different layers. Just as a warm coat might have a smooth lining, a thick and bulky interlining, and an outer layer of a third fabric, so the heart wall has three tissue layers (Fig. 10-2). Starting with the innermost layer, these are as follows:
* The endocardium is a thin, smooth layer of epithelial cells that lines the heart’s interior. The endocardium provides a smooth surface for easy flow as blood travels through the heart. Extensions of this membrane cover the flaps (cusps) of the heart valves.
* The myocardium, the heart muscle, is the thickest layer and pumps blood through the vessels. Cardiac muscle’s unique structure is described in more detail next.
* The epicardium is a serous membrane that forms the thin, outermost layer of the heart wall.
The Pericardium
The pericardium is the sac that encloses the heart (Fig. 10-2). The outermost and heaviest layer of this sac is the fibrous pericardium. Connective tissue anchors this pericardial layer to the diaphragm, located inferiorly; the sternum, located anteriorly; and to other structures surrounding the heart, thus holding the heart in place.

Figure 10-2 Layers of the heart wall and pericardium. The serous pericardium covers the heart and lines the fibrous pericardium.
A serous membrane lines this fibrous sac and folds back at the base to cover the heart’s surface. Anatomically, the outer layer of this serous membrane is called the parietal layer, and the inner layer is the visceral layer, also known as the epicardium, as previously noted. A thin film of fluid between these two layers reduces friction as the heart moves within the pericardium. Normally the visceral and parietal layers are very close together, but fluid may accumulate in the region between them, the pericardial cavity, under certain disease conditions.
Cardiac muscle cells are lightly striated (striped) based on alternating actin and myosin filaments, as seen in skeletal muscle cells. Unlike skeletal muscle cells, however, cardiac muscle cells have a single nucleus instead of multiple nuclei. Also, cardiac muscle tissue is involuntarily controlled. There are specialized partitions between cardiac muscle cells that show faintly under a microscope (Fig. 10-3). These intercalated disks are actually modified plasma membranes that firmly attach adjacent cells to each other but allow for rapid transfer of electrical impulses between them. The adjective intercalated is from Latin and means “inserted between.” Another feature of cardiac muscle tissue is the branching of the muscle fibers (cells). These fibers are interwoven so that the stimulation that causes the contraction of one fiber results in the contraction of a whole group. The intercalated disks and the branching cellular networks allow cardiac muscle cells to contract in a coordinated manner.
Divisions of the Heart
Healthcare professionals often refer to the right heart and the left heart, because the human heart is really a double pump (Fig. 10-4). The right side pumps blood low in oxygen to the lungs through the pulmonary circuit. The left side pumps oxygenated blood to the remainder of the body through the systemic circuit. Each side of the heart is divided into two chambers.
Special Features of the Myocardium
Cardiac muscle cells are lightly striated (striped) based on alternating actin and myosin filaments, as seen in skeletal muscle cells. Unlike skeletal muscle cells, however, cardiac muscle cells have a single nucleus instead of multiple nuclei. Also, cardiac muscle tissue is involuntarily controlled. There are specialized partitions between cardiac muscle cells that show faintly under a microscope (Fig. 10-3). These intercalated disks are actually modified plasma membranes that firmly attach adjacent cells to each other but allow for rapid transfer of electrical impulses between them. The adjective intercalated is from Latin and means “inserted between.” Another feature of cardiac muscle tissue is the branching of the muscle fibers (cells). These fibers are interwoven so that the stimulation that causes the contraction of one fiber results in the contraction of a whole group. The intercalated disks and the branching cellular networks allow cardiac muscle cells to contract in a coordinated manner.
Divisions of the Heart
Healthcare professionals often refer to the right heart and the left heart, because the human heart is really a double pump (Fig. 10-4). The right side pumps blood low in oxygen to the lungs through the pulmonary circuit. The left side pumps oxygenated blood to the remainder of the body through the systemic circuit. Each side of the heart is divided into two chambers.
Four Chambers
The upper chambers on the right and left
Figure 10-3 Cardiac muscle tissue viewed under the microscope (x540). The sample shows light striations (arrowheads), intercalated disks, and branching fibers (arrow).
sides, the atria, are mainly blood-receiving chambers (Fig. 10-5). The lower chambers on the right and left side, the ventricles are forceful pumps. The chambers, listed in the order in which blood flows through them, are as follows:
1. The right atrium is a thin-walled chamber that receives the blood returning from the body tissues. This blood, which is low in oxygen, is carried in veins, the blood vessels leading back to the heart from the body tissues. The superior vena cava brings blood from the head, chest, and arms; the inferior vena cava delivers blood from the trunk and legs. A third vessel that opens into the right atrium brings blood from the heart muscle itself.
2. The right ventricle pumps the venous blood received from the right atrium to the lungs. It pumps into a large pulmonary trunk, which then divides into right and left pulmonary arteries, which branch to the lungs. An artery is a vessel that takes blood from the heart to the tissues. Note that the pulmonary arteries in Figure 10-5 are colored blue because they are carrying deoxygenated blood, unlike other arteries, which carry oxygenated blood.
3. The left atrium receives blood high in oxygen content as it returns from the lungs in pulmonary veins. Note that the pulmonary veins in Figure 10-5 are colored red because they are carrying oxygenated blood, unlike other veins, which carry deoxygenated blood.
4. The left ventricle, which is the chamber with the thickest wall, pumps oxygenated blood to all parts of the body. This blood goes first into the aorta, the largest artery, and then into the branching systemic arteries that take blood to the tissues. The heart’s apex, the lower pointed region, is formed by the wall of the left ventricle (see Fig. 10-2).
2. The right ventricle pumps the venous blood received from the right atrium to the lungs. It pumps into a large pulmonary trunk, which then divides into right and left pulmonary arteries, which branch to the lungs. An artery is a vessel that takes blood from the heart to the tissues. Note that the pulmonary arteries in Figure 10-5 are colored blue because they are carrying deoxygenated blood, unlike other arteries, which carry oxygenated blood.
3. The left atrium receives blood high in oxygen content as it returns from the lungs in pulmonary veins. Note that the pulmonary veins in Figure 10-5 are colored red because they are carrying oxygenated blood, unlike other veins, which carry deoxygenated blood.
4. The left ventricle, which is the chamber with the thickest wall, pumps oxygenated blood to all parts of the body. This blood goes first into the aorta, the largest artery, and then into the branching systemic arteries that take blood to the tissues. The heart’s apex, the lower pointed region, is formed by the wall of the left ventricle (see Fig. 10-2).

Figure 10-4 The heart as a double pump. The right side of the heart pumps blood through the pulmonary circuit to the lungs to be oxygenated; the left side of the heart pumps blood through the systemic circuit to all other parts of the body.

Figure 10-5 The heart and great vessels.
The heart’s chambers are completely separated from each other by partitions, each of which is called a septum. The interatrial septum separates the two atria, and the interventricular septum separates the two ventricles. The septa, like the heart wall, consist largely of myocardium.
* The right atrioventricular (AV) valve is also known as the tricuspid valve because it has three cusps, or flaps, that open and close. When this valve is open, blood flows freely from the right atrium into the right ventricle. When the right ventricle begins to contract, however, the valve is closed by blood squeezed backward against the cusps. With the valve closed, blood cannot return to the right atrium but must flow forward into the pulmonary arterial trunk.
* The left atrioventricular (AV) valve is the bicuspid valve, but it is commonly referred to as the mitral valve (named for a miter, the pointed, two-sided hat worn by bishops).
Four Valves
One-way valves that direct blood flow through the heart are located at the entrance and exit of each ventricle (Fig. 10-6). The entrance valves are the atrioventricular (AV) valves, so named because they are between the atria and ventricles. The exit valves are the semilunar valves, so named because each flap of these valves resembles a half-moon. Each valve has a specific name, as follows:* The right atrioventricular (AV) valve is also known as the tricuspid valve because it has three cusps, or flaps, that open and close. When this valve is open, blood flows freely from the right atrium into the right ventricle. When the right ventricle begins to contract, however, the valve is closed by blood squeezed backward against the cusps. With the valve closed, blood cannot return to the right atrium but must flow forward into the pulmonary arterial trunk.
* The left atrioventricular (AV) valve is the bicuspid valve, but it is commonly referred to as the mitral valve (named for a miter, the pointed, two-sided hat worn by bishops).
It has two heavy cusps that permit blood to flow freely from the left atrium into the left ventricle. The cusps close when the left ventricle begins to contract; this closure prevents blood from returning to the left atrium and ensures the forward flow of blood into the aorta. Both the right and left AV valves are attached by means of thin fibrous threads to muscles in the walls of the ventricles. The function of these threads, called the chordae tendineae (see Fig. 10-6), is to stabilize the valve flaps when the ventricles contract so that the force of the blood will not push them up into the atria. In this manner, they help to prevent a backflow of blood when the heart beats.
* The pulmonary valve, also called the pulmonic valve, is a semilunar valve located between the right ventricle and the pulmonary trunk that leads to the lungs.
* The pulmonary valve, also called the pulmonic valve, is a semilunar valve located between the right ventricle and the pulmonary trunk that leads to the lungs.
As soon as the right ventricle begins to relax from a contraction, pressure in that chamber drops. The higher pressure in the pulmonary artery, described as back pressure, closes the valve and prevents blood from returning to the ventricle.
* The aortic valve is a semilunar valve located between the left ventricle and the aorta. After contraction of the left ventricle, back pressure closes the aortic valve and prevents the back flow of blood from the aorta into the ventricle.
Figure 10-7 traces a drop of blood as it completes a full circuit through the heart’s chambers. Note that blood passes through the heart twice in making a trip from the heart’s right side through the pulmonary circuit to the lungs and back to the heart’s left side to start on its way through the systemic circuit. Although Figure 10-7 follows the path of a single drop of blood in sequence through the heart, the heart’s two sides function in unison to pump blood through both circuits at the same time.
Blood Supply to the Myocardium
Only the endocardium comes into contact with the blood that flows through the heart chambers. Therefore, the myocardium must have its own blood vessels to provide oxygen and nourishment and to remove waste products. Together, these blood vessels provide the coronary circulation. The main arteries that supply blood to the muscle of the heart are the right and left coronary arteries (Fig. 10-8), named because they encircle the heart like a crown. These arteries, which are the first to branch off the aorta, arise just above the cusps of the aortic valve and branch to all regions of the heart muscle. They receive blood when the heart relaxes because the aortic valve must be closed to expose the entrance to these vessels (Fig. 10-9). After passing through capillaries in the myocardium, blood drains into a system of cardiac veins that brings blood back toward the right atrium. Blood finally collects in the coronary sinus, a dilated vein that opens into the right atrium near the inferior vena cava (see Fig. 10-8).
* The aortic valve is a semilunar valve located between the left ventricle and the aorta. After contraction of the left ventricle, back pressure closes the aortic valve and prevents the back flow of blood from the aorta into the ventricle.
Figure 10-7 traces a drop of blood as it completes a full circuit through the heart’s chambers. Note that blood passes through the heart twice in making a trip from the heart’s right side through the pulmonary circuit to the lungs and back to the heart’s left side to start on its way through the systemic circuit. Although Figure 10-7 follows the path of a single drop of blood in sequence through the heart, the heart’s two sides function in unison to pump blood through both circuits at the same time.
Blood Supply to the Myocardium
Only the endocardium comes into contact with the blood that flows through the heart chambers. Therefore, the myocardium must have its own blood vessels to provide oxygen and nourishment and to remove waste products. Together, these blood vessels provide the coronary circulation. The main arteries that supply blood to the muscle of the heart are the right and left coronary arteries (Fig. 10-8), named because they encircle the heart like a crown. These arteries, which are the first to branch off the aorta, arise just above the cusps of the aortic valve and branch to all regions of the heart muscle. They receive blood when the heart relaxes because the aortic valve must be closed to expose the entrance to these vessels (Fig. 10-9). After passing through capillaries in the myocardium, blood drains into a system of cardiac veins that brings blood back toward the right atrium. Blood finally collects in the coronary sinus, a dilated vein that opens into the right atrium near the inferior vena cava (see Fig. 10-8).

Figure 10-6 Valves of the heart (superior view from anterior, atria removed). (A) When the heart is relaxed (diastole), the AV valves are open and blood flows freely from the atria to the ventricles. The pulmonary and aortic valves are closed. (B) When the ventricles contract, the AV valves close and blood pumped out of the ventricles opens the pulmonary and aortic valves.

Figure 10-7 Pathway of blood through the heart. Blood from the systemic circuit enters the right atrium (1) through the superior and inferior venae cavae, flows through the right AV (tricuspid) valve (2), and enters the right ventricle (3). The right ventricle pumps the blood through the pulmonary (semilunar) valve (4) into the pulmonary trunk, which divides to carry blood to the lungs in the pulmonary circuit. Blood returns from the lungs in the pulmonary veins, enters the left atrium (5), and flows through the left AV (mitral) valve (6) into the left ventricle (7). The left ventricle pumps the blood through the aortic (semilunar) valve (8) into the aorta, which carries blood into the systemic circuit.
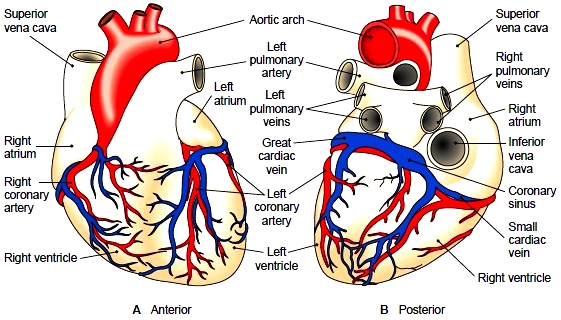
Figure 10-8 Blood vessels that supply the myocardium. Coronary arteries and cardiac veins are shown. (A) Anterior view. (B) Posterior view.

Figure 10-9 Opening of coronary arteries in the aortic valve (anterior view). (A) When the left ventricle contracts, the aortic valve opens. The valve cusps prevent filling of the coronary arteries. (B) When the left ventricle relaxes, backflow of blood closes the aortic valve and the coronary arteries fill.
Contacts: lubopitno_bg@abv.bg www.encyclopedia.lubopitko-bg.com Corporation. All rights reserved.
DON'T FORGET - KNOWLEDGE IS EVERYTHING!